About University of Turin
University of Turin
Articles by University of Turin
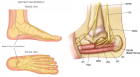
Achilles Tendon Injuries: Comparison of Different Conservative and Surgical Treatment and Rehabilitation
Published on: 21st February, 2017
OCLC Number/Unique Identifier: 7286357861
Despite its high incidence and the great development of literature, there is still controversy about the optimal management of Achilles tendon rupture. The several techniques proposed to treat acute ruptures can essentially be classified into: conservative management (cast immobilization or functional bracing), open repair, minimally invasive technique and percutaneous repair with or without augmentation. Although chronic ruptures represent a different chapter, the ideal treatment seems to be surgical too (debridement, local tissue transfer, augmentation and synthetic grafts). In this paper we reviewed the literature on acute injuries.
Novel European Asiatic Clinical, Laboratory, Molecular and Pathobiological (2015-2020 CLMP) criteria for JAK2V617F trilinear polycythemia vera (PV), JAK2exon12 PV and JAK2V617F, CALR and MPL515 thrombocythemias: From Dameshek to Constantinescu-Vainchenker, Kralovics and Michiels
Published on: 3rd April, 2020
OCLC Number/Unique Identifier: 8576367174
The Myeloproliferative Neoplasms (MPN) of trilinear polycythemia vera (PV) and megakaryocytic leukemia (ML = primary megakaryocytic granulocytic myeloproliferation: PMGM) and Essential Thrombocythemia (ET) in the studies of Dameshek and Michiels are caused by the MPN driver mutations JAK2V617F, JAK2exon12, CALR and MPL515 discovered by Constantinescu-Vainchenker, Green and Kralovics. The JAK2V617F mutated trilinear myeloproliferative neoplasms (MPN) include a broad spectrum of clinical laboratory and bone marrow features in essential thrombocythemia (ET), prodromal PV and erythrocythemic PV, classical PV and advanced stages of masked PV and PV complicated by splenomegaly and secondary myelofibrosis (MF). Heterozygous JAK2V617F mutated ET is associated with low JAK2 allele and MPN disease burden and normal life expectance. In combined heterozygous and homozygous or homozygous JAK2V617F mutated trilinear PV, the JAK2 mutation load increases from less than 50% in prodromal PV and classical PV to above 50% up to 100% in hypercellular PV, advanced PV and PV with MF. Bone marrow histology show diagnostic features of eryhrocytic, megakaryocytic and granulocytic (EMG) myeloproliferation in JAK2V617F mutated trilinear MPN, which clearly differs from monolinear megakaryocytic (M) myelproliferation in MPL and CALR thrombocythemia and dual megakaryocytic granulocytic (MG) myeloproliferation in CALR mutated thrombocythemia. The morphology of clustered large pleomorphic megakaryocytes with hyperlobulated nuclei are similar in JAK2V617F thrombocythemia, prodromal PV and classical PV patients. Monolinear megakaryocytic (M) myeloproliferation of large to giant megakaryocytes with hyperlobulated staghorn-like nuclei is the hallmark of MPL515 mutated normocellular thrombocythemia. CALR mutated thrombocythemia usually presents with high platelet count around 1000x109/l and normocellular megakaryocytic (M) proliferation of immature megakaryocytes with cloud-like hyperchromatic nuclei followed by dual megakaryocytic granulocytic (MG) myeloproliferation followed by various degrees of bone marrow fibrosis. Natural history and life expectancy of MPN patients are related to the response to treatment and the degree of anemia, splenomegaly, myelofibrosis and constitutional symptoms. The acquisition of epigenetic mutations at increasing age on top of MPN disease burden independently predict unfavorable outcome in JAK2V617F, MPL515 and CALR mutated myeloproliferative neoplasms (MPNs, which mutually exclude each other).
RV Function by cardiac magnetic resonance and its relationship to RV longitudinal strain and neutrophil/lymphocyte ratio in patients with acute inferior ST-segment elevation myocardial infarction undergoing primary percutaneous intervention
Published on: 23rd November, 2021
OCLC Number/Unique Identifier: 9359437609
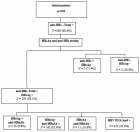
Background: Although acute inferior myocardial infarction (MI) is usually regarded as being lower risk compared with acute anterior MI, right ventricular (RV) myocardial involvement (RVMI) may show an increased risk of cardiovascular (CV) morbidity and mortality in patients with inferior MI. CMR is ideal for assessing the RV because it allows comprehensive evaluation of cardiovascular morphology and physiology without most limitations that hinder alternative imaging modalities. Objectives: To evaluate the sensitivity of strain and strain rate of the RV using 2D speckle tracking echo and the neutrophil/ lymphocyte ratio (NLR) compared to cardiac MRI (CMR) as the gold standard among patients with inferior STEMI undergoing primary percutaneous coronary intervention (PCI). Methodology: 40 Patients with inferior MI who had primary PCI were included in the study; they were divided into two groups according to the RVEF using CMR. NLR was done in comparison to RVEF.Results: out of the 40 patients, 18 (45%) patients had RV dysfunction. 2D echocardiography was done for all patients, where fractional area change (FAC) in the RV dysfunction group appeared to be significantly reduced compared to the group without RV dysfunction (p value = 0.03). In addition, RV longitudinal strain (LS) by speckle tracking echo was reduced with an average of 19.5 ± 3.9% in the RV dysfunction group.Both CMR- derived RV SV, and EF were lower among the RV dysfunction group, (26.8 ± 15.8) ml and (35.4 ± 6.9)% respectively, with large RV systolic volume, with a highly statistically significant difference in comparison to the other group (p value = 0.000). Complications, heart block was significantly higher in patients with RV dysfunction (p value = 0.008) as it occurred in 5 (27.8%) patients.N/L ratio for predicting RV dysfunction by CMR had a cut-off value of > 7.7 with low sensitivity (38.8%) and high specificity (77.3 %). In contrast, LS for predicting RV dysfunction by CMR had high sensitivity (83.3%) and high specificity (63.6%) with p value = 0.005.Conclusion: Our results showed that RV dysfunction in inferior MI is better detected using cardiac magnetic resonance imaging. In inferior STEMI patients who underwent primary PCI, NLR has low sensitivity but high specificity for predicting RVD when measured by cardiac MRI.

HSPI: We're glad you're here. Please click "create a new Query" if you are a new visitor to our website and need further information from us.
If you are already a member of our network and need to keep track of any developments regarding a question you have already submitted, click "take me to my Query."